
Hospital renovation cost per room in 2026 is a critical metric for hospital leaders who must balance clinical quality, patient experience, and financial performance. Understanding how each component of a renovation contributes to the per‑room budget allows administrators to make smarter, data‑driven decisions.
1. Why Hospital Renovation Cost Per Room Matters in 2026
In 2026, hospital renovation cost per room is no longer just a construction line item—it is a strategic investment that directly affects patient outcomes, staff satisfaction, and long‑term efficiency. As patient expectations rise and healthcare systems face tighter margins, a clear view of per‑room costs helps decision‑makers allocate resources where they have the greatest impact.
1.1 Rising patient expectations and safety standards
Patients and families increasingly expect clean, quiet, comfortable, and technology‑enabled environments that support healing and privacy. At the same time, hospitals must comply with strict safety and accessibility standards, from life‑safety codes to accessibility regulations. These expectations and requirements drive up the complexity and therefore the cost per room.
1.2 Impact on operational efficiency and revenue
Well‑designed rooms can reduce nurse walking time, streamline workflows, and minimize errors, improving productivity and lowering operating expenses. Better‑equipped and more comfortable rooms can also justify higher reimbursement levels or private‑room premiums, directly influencing revenue. When administrators understand cost per room, they can measure renovation ROI more precisely.
1.3 Regulatory and accreditation requirements driving renovation
Regulatory bodies and accreditation organizations continuously update requirements for infection control, medical gas systems, power and data infrastructure, and life‑safety systems. Hospitals that delay renovation may face compliance risks, operational disruptions, or penalties. Factoring these evolving standards into per‑room renovation budgets is essential for long‑term sustainability.
2. Average Hospital Renovation Cost Per Room in 2026
Every hospital is unique, but administrators still need realistic benchmarks to start building budgets. In 2026, average hospital renovation cost per room typically ranges from modest refresh projects to highly complex, technology‑intensive upgrades involving major infrastructure changes.

2.1 Typical cost range per room
A light refresh of a standard patient room focused on finishes and furniture sits at the lower end of the spectrum. Upgrading an older ward with new MEP (mechanical, electrical, plumbing), medical gases, and integrated technology pushes costs toward the higher end. Critical‑care rooms and operating rooms usually sit above standard patient rooms because of specialized systems, equipment, and compliance demands.
2.2 Cost breakdown: construction, systems, furniture, equipment
A typical per‑room renovation budget can be broken down into several major categories:
- Construction and finishes (walls, ceilings, flooring, doors, windows)
- MEP and life‑safety systems (HVAC, medical gases, power, lighting, sprinklers)
- IT and low‑voltage systems (data, nurse call, monitoring, communications)
- Furniture and fixtures (beds, casework, seating, storage)
- Medical equipment and accessories
- Design, project management, and permitting
- Contingency for unknowns
A typical hospital renovation budget per room can be summarized as follows.
| Cost Category | Typical Components | Relative Impact on Per Room Cost | Key Considerations |
|---|---|---|---|
| Construction & finishes | Walls, ceilings, flooring, doors, windows, wall protection | Medium to high | Drives visual impact and durability |
| MEP & life‑safety systems | HVAC, medical gases, power, lighting, sprinklers, alarms | High | Often significant in older buildings |
| IT & low‑voltage systems | Data, nurse call, monitoring, communications | Medium | Requires careful integration with existing infrastructure |
| Furniture & fixtures | Beds, casework, seating, storage, overbed tables | Medium | Balances comfort, workflow, and infection control |
| Medical equipment & accessories | Monitors, IV poles, booms, task lighting | Medium to high | Varies widely by room type and care model |
| Design, project management & permitting | Professional fees, coordination, approvals, inspections | Low to medium | Essential for compliance and risk control |
| Contingency | Allowance for unknowns and scope changes | Variable | Protects the project from unexpected costs |
2.3 Cost per room by hospital type
Different hospital types face different cost pressures. Community hospitals may focus on cost‑effective upgrades that improve comfort and basic technology. Teaching hospitals often require more infrastructure for education and research, increasing per‑room complexity. Specialty hospitals, such as cardiac or oncology centers, frequently invest more in equipment‑intensive rooms that demand robust structural and technological support.
3. Key Factors Influencing Hospital Renovation Costs per Room
Beyond simple square footage, a range of factors influences renovation cost per room. Understanding these drivers helps avoid underestimation and costly surprises later in the project.
3.1 Room type and clinical complexity
General patient rooms, ICU rooms, emergency department bays, operating rooms, and procedure rooms all have different clinical requirements. A typical medical‑surgical room requires basic monitoring and support utilities, while ICU and OR spaces require higher redundancy, more integrated equipment, and stricter environmental controls. The more complex the room type, the higher the per‑room cost.
3.2 Structural and MEP upgrades
Older buildings often lack the structural capacity and conduit pathways needed for modern systems. Adding new HVAC units, medical gas lines, or upgraded power and data may require structural reinforcement, slab work, or rerouting existing infrastructure. These hidden structural and MEP upgrades can significantly increase per‑room renovation costs.
3.3 Infection control and hygiene requirements
Hospitals must design rooms to support rigorous infection‑control protocols. This often means using non‑porous, easy‑to‑clean materials, seamless flooring, coved bases, and carefully detailed joints. Negative‑pressure or isolation rooms require specialized ventilation strategies and monitoring. Infection‑control design features can raise initial costs but protect patient safety and reduce long‑term risks.
3.4 Technology integration
Modern hospital rooms typically integrate nurse call systems, EMR access points, bedside monitoring, smart lighting, and sometimes telehealth capabilities. Coordinating these technologies across power, data, wall systems, and furniture adds design and installation complexity. The level of integration chosen has a direct impact on cost per room.
3.5 Location, labor costs, and supply chain
Regional labor rates, local construction markets, and supply‑chain conditions all affect renovation costs. Urban hospitals with limited access or phasing constraints may see higher labor premiums. Global events that affect raw materials, transportation, or manufacturing lead times can also influence the cost and availability of furniture and equipment.
4. Hospital Furniture and Fixtures: Cost Per Room in 2026
Furniture and fixtures play a critical role in both the functionality and the perception of a hospital room. In 2026, hospital furniture cost per room is driven by clinical needs, durability requirements, user comfort, and infection‑control standards.

4.1 Core furniture items per room
Most patient rooms include a consistent set of furniture elements: an adjustable patient bed, bedside cabinet, overbed table, visitor or family seating, and built‑in or freestanding storage for personal items and clinical supplies. Staff seating, charting surfaces, and integrated wall panels or headwalls may also be part of the furniture package.
4.2 Medical‑grade materials and cost implications
Hospital furniture must withstand frequent cleaning, disinfectants, and heavy daily use. Medical‑grade materials such as antimicrobial laminates, moisture‑resistant cores, powder‑coated steel frames, and high‑performance upholstery carry higher upfront costs than standard commercial materials. However, they usually deliver longer lifespans, lower maintenance costs, and enhanced infection‑control performance.
4.3 Typical furniture cost ranges per room
Furniture cost per room varies depending on the room type and the quality level selected. Standard patient rooms may prioritize robust, value‑driven solutions that support comfort and easy maintenance. ICU and specialty rooms often require more specialized beds, integrated equipment rails, and customized storage solutions that increase cost per room. Thoughtful standardization of furniture packages across similar room types can help control these costs.
4.4 Balancing upfront cost, durability, and maintenance
The most cost‑effective approach looks beyond initial price tags and considers total cost of ownership. Durable designs that resist damage, are easy to clean, and minimize replacement cycles can reduce lifetime cost per room. Partnering with specialized healthcare furniture manufacturers, such as HongYe Healthcare Furniture , helps hospitals select solutions tailored to clinical workflows, infection‑control needs, and long‑term budget constraints. HY Healthcare Furniture focuses on medical‑grade materials, ergonomic design, and project‑based customization, enabling hospitals to optimize both quality and per‑room costs in renovation projects.
5. Medical Equipment and Technology: Budgeting Beyond Furniture
Furniture is only part of the room; medical equipment and technology are equally important for budgeting. Ignoring these categories early in planning can cause serious budget gaps.
5.1 Basic equipment per patient room
Even a standard patient room requires a minimum equipment set: vital‑sign monitoring, IV poles or integrated infusion supports, medical gas outlets, adequate clinical lighting, and nurse call interfaces. These items must be coordinated with the room’s utilities and furniture layouts to ensure safe, efficient care delivery.
5.2 Additional costs in ICU and specialty rooms
ICU rooms, step‑down units, and specialized treatment rooms typically include more advanced monitoring, multiple infusion devices, ceiling‑mounted booms or lifts, and backup systems. These additions significantly raise the equipment cost per room and often demand enhanced structural and MEP design. When estimating ICU renovation costs, it is crucial to include both the direct price of equipment and the indirect costs of infrastructure to support it.
5.3 Integration with existing hospital systems
New equipment must connect seamlessly with existing IT networks, EMR platforms, alarm‑management systems, and building‑management systems. Integration work—such as software configuration, interface development, and testing—can add meaningful cost. Planning for these integration expenses at the per‑room level avoids budget surprises late in the project.
6. Sample Per Room Budgets for Different Hospital Renovation Scenarios
Because every project has its own scope, presenting a few typical renovation scenarios helps stakeholders visualize how per‑room costs stack up.

6.1 Light refresh: finishes and furniture upgrade only
A light refresh focuses on improving the look and feel of the room without major infrastructure changes. This scenario typically includes new paint, flooring, wall protection, upgraded lighting fixtures, and updated hospital furniture. It is ideal for functional rooms that are structurally sound but visually outdated.
6.2 Mid‑level renovation: finishes + MEP adjustments + new furniture
A mid‑level renovation combines a cosmetic refresh with targeted upgrades to HVAC, power, lighting, and medical gas outlets where needed. It often includes new hospital‑grade furniture and more integrated headwall or casework solutions. This scope is common when hospitals want to modernize patient experience and better support staff workflows without fully rebuilding systems.
6.3 Full renovation: structural changes + MEP overhaul + full equipment update
In a full renovation scenario, rooms are reconfigured, walls may be relocated, and MEP and life‑safety systems are comprehensively upgraded. New medical equipment, smart‑room technology, and fully customized furniture and millwork are installed. Although the per‑room cost is highest in this scenario, it can transform an aging ward into a state‑of‑the‑art unit that supports advanced care models.
6.4 Cost comparison by scenario
The matrix below compares three typical renovation scenarios and their impact on per room cost and operations.
| Renovation Scenario | Typical Scope | Impact on Operations | Indicative Per Room Cost Level | When to Consider |
|---|---|---|---|---|
| Light refresh | New finishes, minor repairs, updated lighting, new furniture | Minimal disruption | Low | Rooms are functional but visually outdated |
| Mid‑level renovation | Finishes, targeted MEP upgrades, new furniture and casework | Moderate disruption, phased work | Medium | Need to modernize comfort and workflows without full rebuild |
| Full renovation | Reconfiguration, major MEP overhaul, new equipment and furniture | Highest disruption, complex phasing | High | Aging infrastructure, new clinical model, or major service change |
7. How to Build a Realistic Hospital Renovation Budget Per Room
Creating a reliable renovation budget per room requires a structured approach. Rushed or oversimplified estimates often lead to overruns and delays.

7.1 Step‑by‑step budgeting process
A practical process includes: defining project goals, identifying all room types involved, developing standard room templates, and assigning cost ranges per room type. Next, project teams add indirect costs such as design fees, permitting, phasing, temporary decanting, and project management. Finally, they review the budget with clinical, facilities, and finance leaders to validate assumptions.
7.2 Recommended contingency percentage
Healthcare renovation projects frequently uncover hidden conditions and unforeseen requirements. Setting aside an appropriate contingency percentage at the project and per‑room level helps manage these uncertainties. Contingency should be clearly separated from base construction and furniture costs so decision‑makers can see how much flexibility remains.
7.3 Coordinating with architects, engineers, and vendors
Accurate per‑room budgeting depends on early collaboration between architects, engineers, construction managers, and key vendors such as furniture and equipment suppliers. Involving these partners early allows more precise quantity take‑offs, better product selections, and realistic lead‑time assumptions. This collaboration reduces the risk of value‑engineering cuts that compromise design intent later.
7.4 Common budgeting mistakes to avoid
Frequent mistakes include underestimating infrastructure upgrades, ignoring integration costs for technology, and assuming “typical” rooms without accounting for specialty spaces. Another common issue is budgeting only for initial purchase prices while ignoring long‑term maintenance and replacement. Recognizing these pitfalls early leads to more reliable per‑room budgets.
8. Choosing the Right Hospital Furniture and Renovation Partners
The choice of partners has a significant impact on renovation outcomes, both financially and clinically. Trusted suppliers and experienced contractors help hospitals stay on budget while achieving design and performance goals.
8.1 Criteria for selecting hospital furniture suppliers
Quality healthcare furniture suppliers offer medical‑grade products, robust warranties, proven project experience, and the ability to support large‑scale rollouts. They should also provide design assistance, detailed shop drawings, and installation support. Clear communication, after‑sales service, and the capacity to handle future expansion are important selection criteria.
8.2 Working with specialized healthcare furniture manufacturers: HY Healthcare Furniture
Partnering with specialized manufacturers like HY Healthcare Furniture gives hospitals access to expertise tailored to clinical environments. HY Healthcare Furniture (www.hyhealthcarefurniture.com) focuses on project‑based healthcare solutions, providing patient‑room furniture, nurse‑station casework, waiting‑area seating, and other medical‑specific furnishings. The company emphasizes infection‑control design, ergonomics, and durability, helping hospitals manage per‑room costs while meeting strict quality and safety standards. Through customized packages and flexible configurations, HY Healthcare Furniture supports hospitals in aligning design, function, and budget across renovation projects.
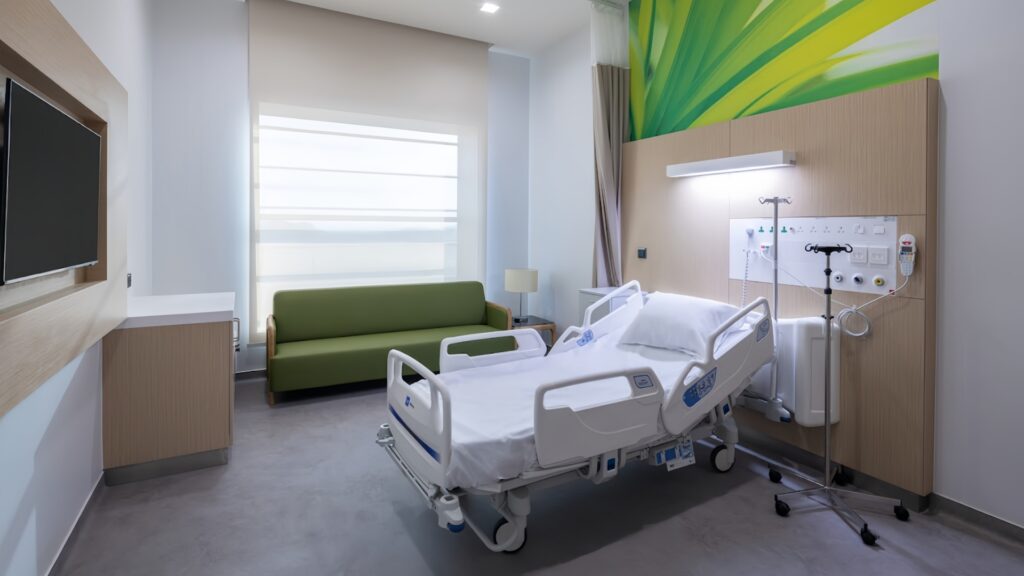
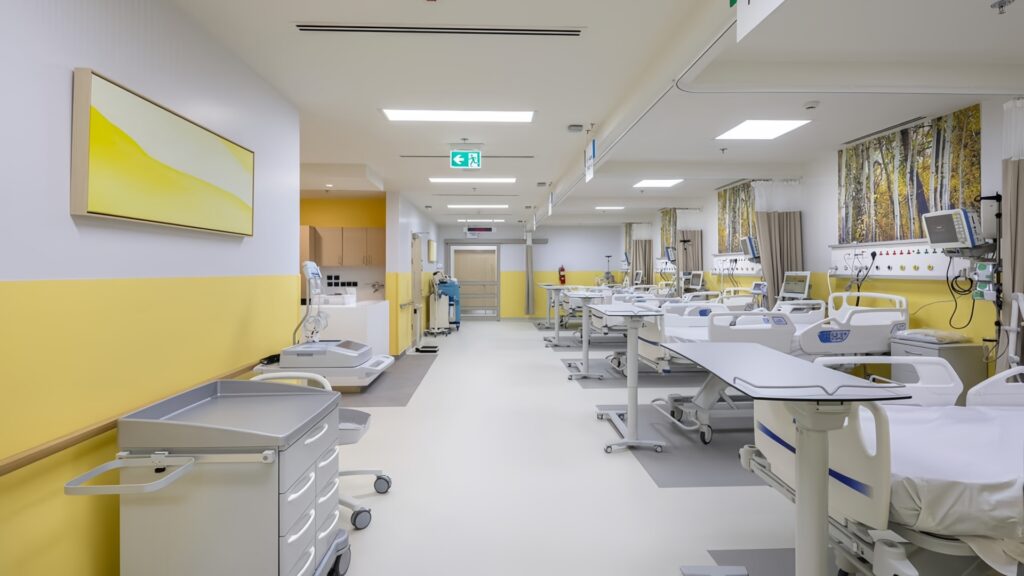
8.3 Case example: Saudi German Hospital Makkah project
A practical example of this approach can be seen in the Saudi German Hospital Makkah medical project, where Hongye Furniture provided a comprehensive furniture solution. In that project, the team worked closely with hospital stakeholders to define functional requirements for different room types, from patient rooms to clinical support areas. Standardized yet customizable furniture packages improved design consistency, simplified installation, and optimized per‑room costs without sacrificing patient comfort or clinical performance.

8.4 Importance of mock‑up rooms and pilot testing
Creating mock‑up rooms before full rollout allows clinical staff to test layouts, furniture, and equipment in real‑world scenarios. Feedback from these pilots can lead to adjustments that improve workflows, safety, and comfort. This iterative process ensures that the final room design is both clinically effective and cost‑efficient.
9. 2026 Trends in Hospital Renovation and Furniture Design
Trends in healthcare design continue to evolve as hospitals respond to new challenges and technologies. Renovation budgets must account for these shifts.
9.1 Patient‑centered and family‑friendly layouts
Hospitals are designing rooms that give patients more control over lighting, privacy, and entertainment, while providing comfortable zones for family members. These changes may require more flexible furniture configurations and thoughtful space planning.
9.2 Sustainability and energy‑efficient materials
Sustainability is increasingly important in healthcare. Low‑VOC finishes, energy‑efficient lighting, and durable materials that extend product lifespans contribute to environmental goals and long‑term cost savings. Furniture choices that support sustainable certifications can also enhance a hospital’s public image.
9.3 Flexible and modular furniture
Modular and reconfigurable furniture allows hospitals to adapt rooms to changing care models without full renovations. For example, modular headwalls, movable casework, and reconfigurable seating support evolving clinical needs. This flexibility can lower lifetime cost per room by reducing future renovation scope.
9.4 Integration of digital health and smart room technology
Smart hospital rooms integrate sensors, automation, and digital tools to improve safety and patient experience. Furniture solutions increasingly accommodate technology through built‑in power, data, and device‑mounting options. Planning for these integrations during renovation prevents expensive retrofits later.
10. Cost‑Saving Strategies Without Compromising Safety and Quality
Cost control does not have to mean cutting corners on safety or patient care. The most effective strategies focus on smarter planning and standardization.

10.1 Standardizing room layouts and furniture packages
Standardizing layouts and furniture across similar room types reduces design time, simplifies installation, and enables bulk purchasing. It also helps staff work more efficiently because they know where to find equipment and supplies in every room.
10.2 Phased renovation to minimize downtime
Phasing renovation work allows hospitals to keep critical services open while upgrading spaces. Thoughtful phasing plans limit revenue loss and reduce the need for expensive temporary facilities. While phasing can add some logistical complexity, it often lowers overall financial impact.
10.3 Leveraging bulk purchasing and long‑term partnerships
Negotiating multi‑project or multi‑year agreements with furniture and equipment suppliers can unlock volume discounts and preferential terms. Long‑term partnerships also improve product consistency and reduce the administrative burden of sourcing for each new project.
10.4 Reusing and refurbishing where safe and compliant
Not all existing elements need to be replaced. When safe and compliant, refurbishing certain furniture items or reusing casework in non‑critical areas can conserve budget. Clear criteria should be established with infection‑control and facilities teams to determine what can be reused.
11. Common Pitfalls in Hospital Room Renovations
Despite careful planning, many hospital renovations encounter avoidable problems. Understanding common pitfalls helps project teams stay ahead of them.
11.1 Underestimating regulatory and inspection requirements
Failing to fully account for regulatory reviews, inspections, and documentation can cause delays and extra costs. Engaging code consultants and involving authorities early in design reduces the risk of rework.
11.2 Ignoring infection control in material selection
Choosing products based solely on initial price without considering infection‑control performance can backfire. Surfaces that are difficult to clean or degrade under harsh disinfectants may require early replacement, increasing long‑term costs.
11.3 Poor coordination between construction and hospital operations
Renovation activities can disrupt clinical services if phasing and communication are weak. Close coordination with nursing leadership, infection‑control teams, and support departments is essential to minimize noise, dust, and access issues.
11.4 Incomplete planning for future technology upgrades
Rooms that lack capacity for additional power, data, or equipment mounting points may require invasive upgrades sooner than expected. Planning for future technology today helps avoid premature renovations and protects the per‑room investment.
12. FAQs: Hospital Renovation Cost Per Room in 2026
How much does it cost to renovate a hospital room in 2026?
Costs vary widely depending on scope, room type, and location, but hospitals should expect a broad range from light cosmetic refreshes to fully reconfigured, technology‑intensive projects. Creating standard room templates for each renovation scenario is the best way to establish realistic per‑room expectations.
The table below illustrates how renovation cost per room varies by clinical room type and scope of work.
| Room Type | Typical Scope of Work | Indicative Renovation Cost Per Room (2026) | Notes |
|---|---|---|---|
| Standard patient room | Finishes, basic MEP adjustments, furniture | Low to medium range | Suitable for light to mid‑level upgrades |
| Private patient room | Finishes, upgraded MEP, enhanced privacy features | Medium range | Often includes more amenities for families |
| ICU room | Finishes, complex MEP, advanced monitoring support | Medium to high range | Higher infrastructure and equipment needs |
| Step‑down / HDU room | Finishes, moderate MEP upgrades, monitoring support | Medium range | Transitional acuity level |
| Operating room | Full MEP upgrade, specialized systems, equipment | Highest range | Most complex clinical environment |
What is the average cost to renovate an ICU room per bed?
ICU rooms typically cost more per bed than standard patient rooms due to additional monitoring equipment, medical gases, and infrastructure needs. Hospitals should allow for higher budgets in critical‑care units and carefully coordinate equipment and MEP requirements in early design phases.
How much should I budget for hospital furniture per room?
Furniture budgets depend on the quality level, room type, and chosen materials. Partnering with specialized healthcare furniture manufacturers, such as HY Healthcare Furniture, helps define realistic per‑room furniture packages that balance performance, aesthetics, and long‑term value.
What percentage of my budget should be reserved as contingency?
Healthcare renovation projects benefit from a dedicated contingency to manage unknowns such as hidden conditions or scope adjustments. Setting a clear contingency percentage at the outset and tracking its use throughout the project supports better decision‑making.
How long does a typical hospital room renovation take?
Timelines depend on scope, phasing, and site constraints. Light refreshes can often be completed relatively quickly, while full renovations with structural and MEP work take longer and may require complex sequencing to keep the hospital operational.
13. Conclusion and Next Steps
Renovating hospital rooms in 2026 requires a careful balance between cost per room, clinical performance, and future flexibility. By understanding the drivers of construction, furniture, and equipment costs, hospital leaders can develop realistic budgets that support both patient care and financial sustainability.
Partnering with experienced healthcare furniture providers such as HY Healthcare Furniture, along with trusted design and construction teams, helps transform renovation plans into efficient, high‑performing spaces. If you are planning a renovation project, consider developing standard room templates, engaging key partners early, and exploring comprehensive furniture solutions that optimize cost per room across your facility.
